COVID-19 infection may be part of a ‘perfect storm’ for Parkinson’s disease
October 21, 2020

GRAND RAPIDS, Mich. (Oct. 22, 2020) — Can COVID-19 infection increase the risk of developing Parkinson’s disease?
That’s the question posed by a new commentary published in the journal Trends in Neurosciences, which explores three known case studies of people developing Parkinson’s-like symptoms in the weeks following infection with SARS-CoV-2, the virus that causes COVID-19. While rare, these cases provide important insights into potential long-term implications of infections.
The commentary was co-authored by Patrik Brundin, M.D., Ph.D., of Van Andel Institute, Avindra Nath, M.D., of the National Institute of Neurological Disorders and Stroke of the National Institutes of Health, and J. David Beckham, M.D., of University of Colorado.
“As we continue to grapple with the COVID-19 pandemic today, we also must consider its implications for the future,” Brundin said. “Evidence is mounting that the side effects of COVID-19 infection, such as inflammation and damage to the vascular system, could lay the foundation for development of Parkinson’s disease. COVID-19 is clearly a major and ongoing public health threat, but the consequences of infection may end up being with us for years and decades to come.”
Parkinson’s disease is a multi-system disorder that begins years or even decades before its hallmark movement-related symptoms appear. Growing evidence suggests Parkinson’s arises from a complex mix of factors that vary from person to person, including age, genetic predisposition, history of infections and exposure to certain environmental factors such as pollution or pesticides.
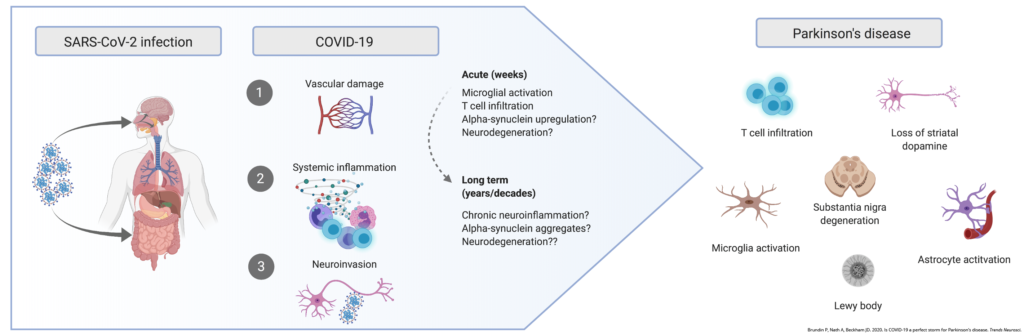
Viral infections in particular may play a role in triggering the earliest stages of Parkinson’s by setting off a cascade that results in the death of brain cells that produce dopamine, a vital chemical messenger whose absence leads to movement issues such as freezing and tremor.
The three cases referenced in the commentary occurred in people without a family history of Parkinson’s and without any known early Parkinson’s symptoms. Two saw an improvement in their Parkinson’s-like symptoms following treatment with traditional Parkinson’s medications that replenish dopamine; the third recovered spontaneously. Although these medications treat symptoms, they often have challenging side effects and do not slow or stop Parkinson’s progression.
“SARS-CoV-2 is considered a respiratory virus, however, its virulence and pathogenic potential particularly for neurological complications continues to surprise us,” Nath said. “Some patients can develop severe neurological manifestations despite mild respiratory symptoms.”
Based on evidence from the case studies and what is known about the mechanisms underpinning Parkinson’s, Brundin, Nath and Beckham suggest three possible ways that COVID-19 infection could contribute to Parkinson’s onset:
- COVID-19 is linked to blood clots and other problems with the vascular system, including in the brain. These vascular insults could cause damage to the area of the brain that produces
dopamine, which subsequently could result in a loss of dopamine that mirrors Parkinson’s. - There is a demonstrated link between chronic inflammation and Parkinson’s. It is possible that severe inflammation resulting from COVID-19 could trigger brain inflammation and cell death
associated with Parkinson’s. - SARS-CoV-2 may be a neurotropic virus, meaning that it attacks the nervous system. Because of this, COVID-19 and Parkinson’s share some early symptoms such as loss of sense of smell and issues with the gut. Additionally, infection with SARS-CoV-2 could lead to an increase in alpha-synuclein, a protein associated with Parkinson’s (this has been seen in other viral infections).
Although these cases do not prove that COVID-19 infection causes Parkinson’s, they do suggest a troubling possible relationship between the virus and subsequent neurodegenerative disorders.
“The large number of respiratory cases due to SARS-CoV2 has allowed us to understand and analyze important neurologic complications of severe respiratory virus infections,” Beckham said. “It is important that we continue our scientific investigations into this new virus so we understand all of the short and long-term complications of the COVID-19 pandemic.”
Going forward, the authors call for long-term studies that follow people who were infected with COVID-19 to monitor them for Parkinson’s development.
Research reported in this publication was supported by Van Andel Institute; the Farmer Family Foundation (Brundin); Division of Intramural Research, National Institute of Neurological Disorders and Stroke of the National Institutes of Health (Nath); and a VA Merit Award (Beckham). The content is solely the responsibility of the authors and does not necessarily represent the official views of the granting organizations.
