Following Parkinson’s footsteps through the brain
For the first time, scientists can monitor the spread of a toxic protein linked to Parkinson’s in a model of the disease in real time. Here’s why that matters.
August 9, 2017

There is still a lot for us to learn when it comes to Parkinson’s disease: How exactly does a healthy cell become sick? Why does this happen? And how can we stop it?
But before those points can be addressed, we need to understand one of the most basic, yet challenging questions in Parkinson’s research—how do we accurately study the disease?
The answer is complicated, so let’s start at the beginning.
Modeling the disease
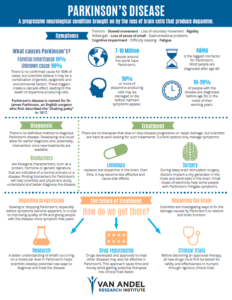
Parkinson’s symptoms stem from the death of brain cells that produce a chemical called dopamine, which plays a major role in our ability to move, among other important functions. People who are eventually diagnosed with the disease often don’t realize something is amiss until they experience tremors, “freezing”, difficulty walking, or another movement-related issue. By the time this happens, much of the damage is already done—around 80 percent of the dopamine-producing cells in the brain may be injured or dead.
Understanding what’s going on behind the scenes is difficult—since it’s happening in the brain, there is no easy way to monitor disease progression or to even definitively diagnose Parkinson’s (there are no blood tests or brain scans that do so). Some answers can be garnered from postmortem studies on brains donated by people with Parkinson’s, but these studies, though important, don’t allow scientists to see what’s happening in real time, especially early in the disease.
Enter a tiny worm called C. elegans, which has a simple nervous system that closely aligns with the more complex human nervous system.
C. elegans may seem humble, but it’s a superstar in neuroscience. It only has about 300 neurons (for comparison, the human brain has about 100 billion), allowing scientists to extensively map and study its entire nervous system, and its short, three-week lifespan makes it a valuable model for studying aging. Since it was first used in the 1960s, C. elegans has contributed to breakthroughs in understanding important biological processes such as development and gene expression as well as many diseases, including Parkinson’s, Alzheimer’s and cancer.
First of its kind
Now, a team at Van Andel Research Institute is hoping a new C. elegans model for Parkinson’s will help them understand one of the disease’s major underlying mechanisms—how toxic alpha-synuclein proteins move from cell to cell.
Clumps of these proteins, called Lewy bodies, are found throughout the brains of people with Parkinson’s, and are thought to cause inflammation, eventually damaging or killing the cell. Growing evidence suggests that a breakdown in cellular energy production shuts down cells’ normal housekeeping functions, allowing these abnormal proteins to accumulate to harmful levels.
The first-of-its-kind model, described this week in Scientific Reports, allows scientists to actually see alpha-synuclein moving from neuron to neuron in C. elegans in a measurable, objective manner. The method is also quick and inexpensive, making it ideal for large-scale studies and screening compounds to see if they can slow or stop the spread of alpha-synuclein.
Already, the team has used the model to show that alpha-synuclein builds up in brain cells as the worms age, and travel down thread-like branches called axons to other cells. What’s more, they’ve also demonstrated that changes in genes that control cellular housekeeping allow the alpha-synuclein to spread faster, adding to the growing evidence that Parkinson’s may be associated with disruptions in energy production systems that keep cells healthy and active.
What does this all mean?
Understanding what’s happening on the most basic level in Parkinson’s disease is an important step in developing ways to slow or stop its progression. This approach also gives scientists a simple, quick way to screen a broad range of promising compounds in an effort to find potentially life-changing treatments.
This study was a collaboration between the laboratories of Dr. Jeremy Van Raamsdonk and Dr. Patrik Brundin in VARI’s Center for Neurodegenerative Science. Research scientist Dr. Trevor Tyson, who started the project six years ago in Brundin’s previous lab at Lund University in Sweden, designed and conducted many of the experiments. Additional authors include Dr. Megan Senchuk, Jason Cooper, Dr. Sonia George, Dr. Jeremy Van Raamsdonk and Dr. Patrik Brundin.
