Making pancreatic cancer treatment personal
November 28, 2016

Pancreatic cancer is one of the most aggressive and difficult to treat cancers, in large part because it usually isn’t detected until it has already spread to other parts of the body.
Furthermore, no two cases of the disease are alike—they vary in their responses to treatment, their molecular makeup and even in their aggressiveness. Current treatments make no distinction between these differences, but what if they could?
This approach, called personalized medicine, has already been successful in other cancers, particularly in breast cancer. Doctors test samples from a person’s tumor and look for specific characteristics called biomarkers that, in this case, indicate if the tumor will response better to drug A or drug B, for example. Although a similar approach doesn’t yet exist for pancreatic cancer, it is well on its way.
Before tumors can be matched up with the most appropriate drug, we must have a better way to definitively diagnose and categorize pancreatic cancer subtypes. While it may sound simple, in reality this is a monumental undertaking that requires in-depth analysis of thousands of potential markers in tumor tissue. Despite the challenges, I’m happy to report we are making significant progress.
Thanks to recent findings, it is clear that pancreatic cancer tumors can be divided using:
- Molecules produced by the cancer cells
- Genetic information
- The amount of cancerous versus non-cancer cells in the tumor (aka the tumor’s makeup)
- How the immune system responds
- The similarity of the cancer cells to certain normal cell types
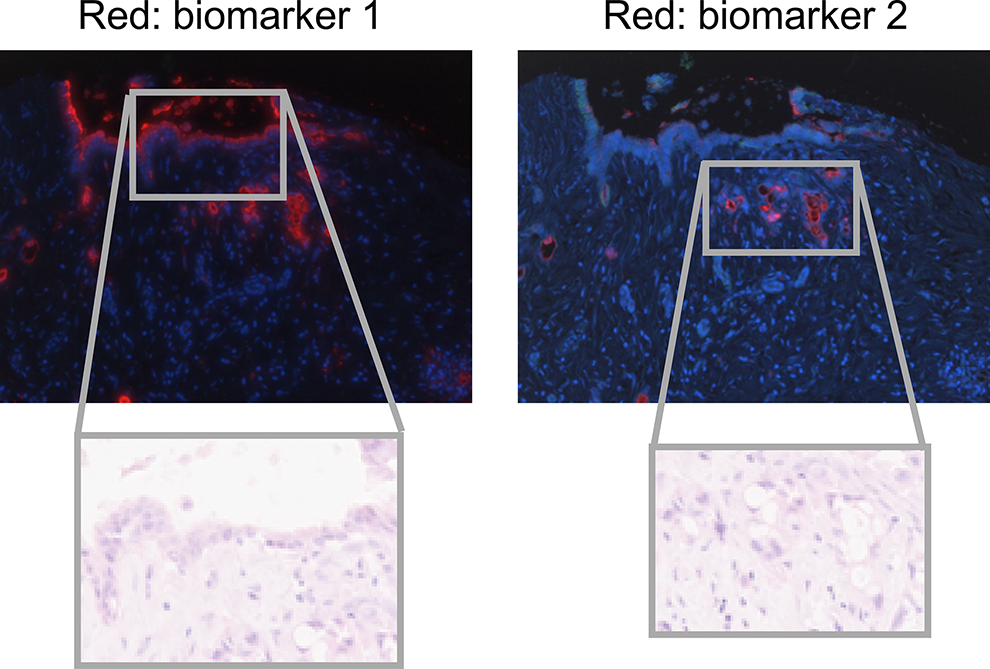
Our research focuses on the first point. Normal cells produce a range of molecules to help carry out their normal function. Cancer cells are no different. Our lab has found that certain carbohydrates are only produced by pancreatic cancer cells, making them ideal biomarker candidates that may aid in an earlier and more definitive diagnosis. We then used this information to develop a blood test that detects 90 percent of pancreatic cancer cases with a low rate of false-positives. We’re now working to refine our method in hopes of bringing this test into the clinic, to help the patients that need it most.
Dr. Brian Haab is an expert in pancreatic cancer. Since he joined Van Andel Research Institute in 2000, his laboratory has significantly contributed to the field’s understanding of biomarkers for the diagnosis and prognosis of the disease. Learn more about Dr. Haab and his work by visiting his website.

