World Heart Day 2016: Four of the coolest things happening in heart disease research
September 29, 2016
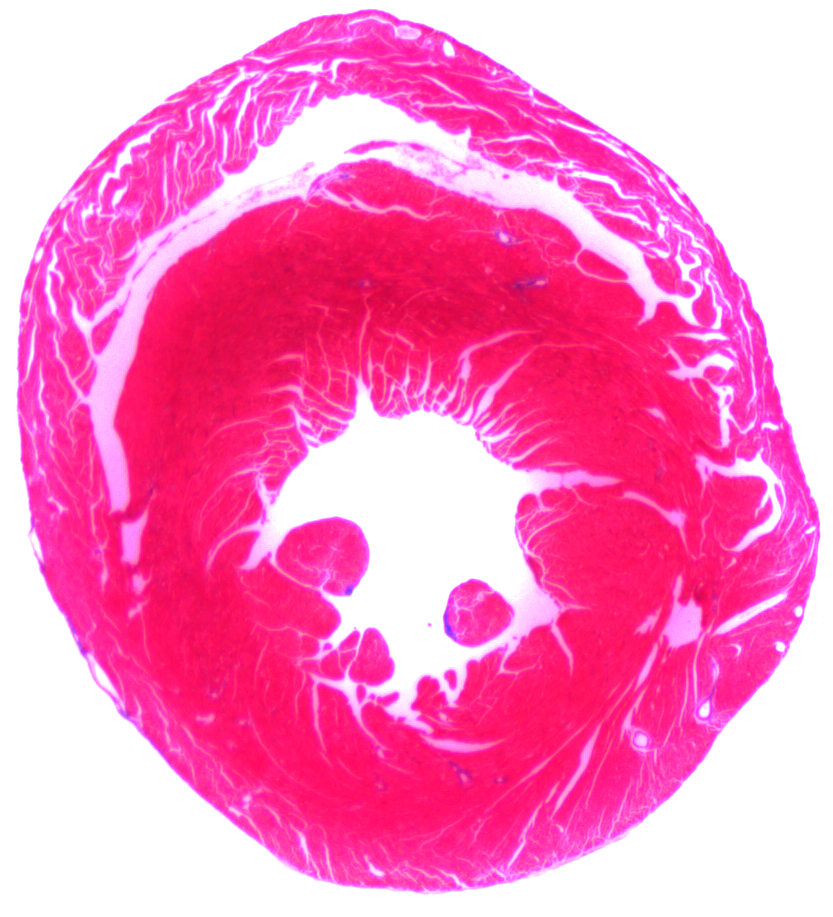
INFOBOX:
- Cardiovascular diseases, such as heart attack and heart failure, are responsible for 31 percent of all deaths, making them the number one cause of death globally, according to the World Health Organization.
- More than 17.5 million people die from cardiovascular diseases annually.
- Not only do many people die of cardiovascular diseases, millions suffer and are left with a disability.
- In the most severe cases, lifelong drug treatment or invasive surgery may be the only treatment options.
Turning blood cells into heart cells. Reading historical signatures in human DNA. Regenerating damaged muscle.
It may sound like science fiction, but for an expert team led by Dr. Stefan Jovinge, it’s reality. He and his group are on the hunt for new ways to treat and repair the damage wrought by heart disease, which claims millions of lives each year. In honor of World Heart Day, we’re taking a look at four of the coolest things happening in Dr. Jovinge’s program. Let’s get started.
History lessons
Did you know we can use genetic traces from nuclear tests of the 20th century to study the heart’s potential to heal itself?
Here’s how it works. The atmosphere contains a radioactive form of carbon called carbon-14, which is incorporated into plants through photosynthesis. Humans then eat the plants (or the animals that eat the plants), ingesting carbon-14 along with their meal, making the carbon-14 content of a person’s body essentially mirror the carbon-14 content of his or her environment. Scientists can measure these carbon levels, allowing them to determine approximate age (read more about how carbon-14 dating works here).
Enter the nuclear tests. Carbon-14 levels in the atmosphere were mostly stable until the nuclear tests during the Cold War era, when they spiked. These events, reflected in people’s DNA in the form of carbon-14, gave scientists a specific moment in time with which to precisely determine age of heart cells. Here’s why that matters—if there was no cellular turnover in the adult heart (that is, the cells weren’t regenerating), one would expect all heart cells in a person to have the same amount of carbon-14. However, Jovinge and his colleagues found the opposite—the cells had variable levels of carbon-14. This work, published in Science in 2009 and expanded with a publication in Cell in 2015, demonstrated what many thought was impossible—that heart muscle cells are naturally regenerating. Which brings us to…
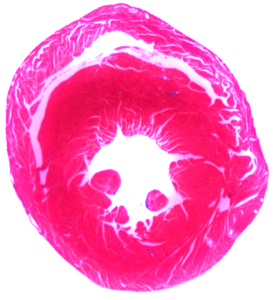
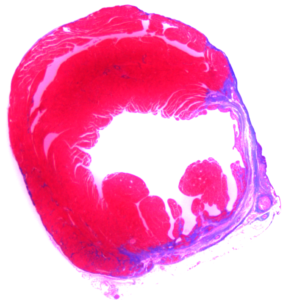
Helping the heart to help itself
Most tissues in the body have the ability to heal following an injury. Think about the skin, for example. If you scrape your knee, you end up with a scab and cool (or embarrassing) story, but eventually the skin grows back. Heart muscle cells, however, are a different story.
For a long time, the prevailing theory held that after a certain point early in life, the heart was incapable of regenerating cells, meaning it could not repair itself after damage such as a heart attack. In 2015, however, Jovinge’s team along with collaborators at Karolinska Institute in Sweden determined that the heart not only has the ability to produce new muscle cells, but that it also experiences cellular turnover throughout a person’s life. They’re now working on ways to promote this process with the aim of finding way to prompt the heart to heal its own injuries.
Reprogramming cells
One of these avenues may lay in the blood, specifically in blood cells that, with some tweaking, can become something wholly different.
Using cutting-edge methods, Jovinge’s team are able to reprogram blood cells, making them revert back to an immature state. Called induced pluripotent stem cells, or IPSCs for short, these cells can then be prompted to become other types of cells, including heart muscle cells. Jovinge and his team will use these cells to bioengineer smart patches that would be placed onto a patient’s heart to stimulate inherent generation and healing of the heart.
A missing link
The heart comprises many different cell types, each with its own function and ability to produce different biological factors. So which one generates the correct factors to stimulate the heart to repair itself?
It’s not quite clear yet but Jovinge and his team are on the trail. They’re looking at individual cells to determine which cells have the best regenerative potential and what about these cells gives them this ability. Finding this source would be a major breakthrough in the field and pave the way for new and better ways to treat heart disease.
Learn more about the exciting work underway as part of the DeVos Cardiovascular Research Program, a joint effort between Van Andel Research Institute and Spectrum Health here.